The 2026 Guide to Medical Billing Denial Codes
MEDICAL CODING


The 2026 Guide to Medical Billing Denial Codes Strategies for Revenue Recovery
In 2026, the U.S. healthcare landscape has reached a tipping point where administrative complexity meets advanced AI-driven payer scrutiny. For healthcare providers, managing medical billing denial codes is no longer just a back-office task—it is a critical strategy for economic survival.
With hospitals and health systems spending billions annually to appeal rejected claims, the cost of "getting it wrong" has never been higher. At Incorpify Solutions, we believe that understanding the "why" behind every denial is the first step toward a healthier bottom line.
Why Claims are Failing
The rise in denial rates are hovering around 15% for private payers and Medicare Advantage is driven by several factors:
Stricter Payer Algorithms: Insurance companies now use real-time AI audits to flag inconsistencies instantly.
Documentation Rigor: Clinical necessity standards have evolved, requiring more granular data for specialized services and telehealth.
Shift in Reimbursement: The transition toward value-based care and bundled payments has introduced new categories of common denial codes in 2026.
Understanding CARC vs. RARC
To fix a claim, you must speak the language of the payer.
CARC (Claim Adjustment Reason Codes): These provide the primary reason for the financial adjustment (e.g., CO-50 for non-covered services).
RARC (Remittance Advice Remark Codes): These provide the necessary context or supplemental instructions needed to resolve the issue.
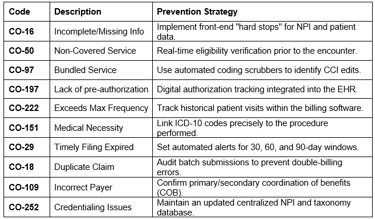
Top 10 Common Denial Codes in 2026
Staying ahead of these frequent culprits can significantly reduce your administrative burden and accelerate cash flow.
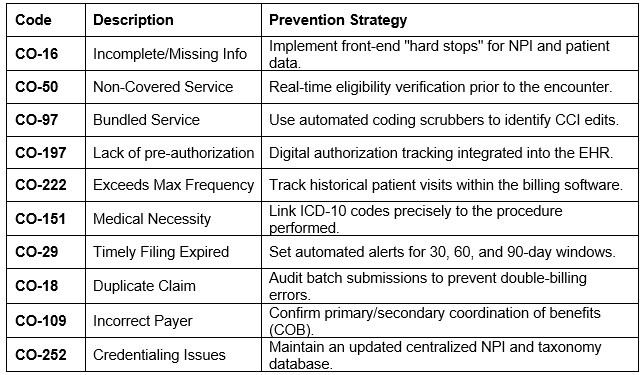

Emerging Trends: Telehealth and AI Audits
The medical billing environment in 2026 has introduced unique challenges, particularly regarding Telehealth and Remote Patient Monitoring (RPM).
Payers are now issuing denials for:
Missing patient consent documentation for virtual visits.
Incorrect "Place of Service" (POS) codes for hybrid care models.
Incomplete quality metrics required for value-based reimbursement.
As payers upgrade their systems, Incorpify Solutions leverages AI-based claim scrubbing to mirror these checks, catching errors before they ever leave your office.
Strategic Denial Management: From Rejection to Recovery
When a denial occurs, a reactive approach is a losing game. A proactive recovery cycle should include:
Root Cause Analysis: Don't just resubmit. Use Denial Management Dashboards to see if specific providers or payers are responsible for recurring patterns.
Professional Appeals: In 2026, appeal letters must be clinical and evidence-based. Cite specific CMS guidelines or payer policy manuals to support medical necessity.
Continuous Coder Training: Coding standards change quarterly. Regular education ensures your team is proficient in the latest modifiers and bundling rules.
Pro Tip: Always analyze CARC and RARC codes together. While the CARC tells you what happened, the RARC often tells you exactly how to fix it.
Secure Your Revenue with Incorpify Solutions
Navigating the complexities of medical billing services in the USA requires more than just software—it requires a partner dedicated to revenue integrity.
Incorpify Solutions combines industry-leading expertise with cutting-edge RCM automation to minimize denials and maximize collections. From real-time eligibility checks to aggressive denial appeals, we ensure your practice stays financially resilient in an ever-changing market.
Ready to reduce your denial rate? Contact Incorpify Solutions today for a comprehensive revenue cycle audit.



